Millions of Americans receive what they believe is good news each year: their cholesterol levels are normal. Armed with reassuring numbers for LDL (“bad” cholesterol), HDL (“good” cholesterol), and triglycerides, they walk away from their doctor’s office confident their heart disease risk is minimal. But this confidence may be dangerously misplaced.
The troubling reality is that heart attacks continue to strike people whose standard cholesterol panels show nothing alarming. This medical paradox has puzzled patients and physicians alike, leading many to question the reliability of conventional cholesterol screening methods.
According to Dr. Seth J. Baum, a leading preventive cardiologist, the answer lies in what traditional blood tests don’t measure—a common inherited cholesterol risk factor that flies under the radar of routine screening.
For decades, the medical establishment has relied on measuring cholesterol levels as the primary indicator of cardiovascular risk. This approach focuses on the amount of cholesterol circulating in the bloodstream, but it misses a crucial piece of the puzzle: the number and characteristics of the particles carrying that cholesterol.
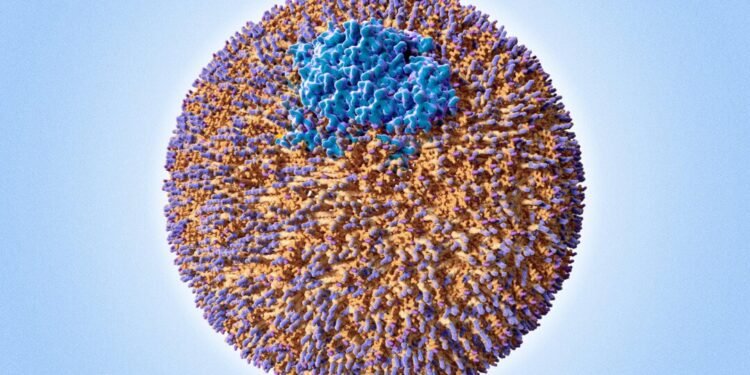
Recent advances in cardiovascular medicine have revealed that apolipoprotein B (apo-B) particle count may offer a far more accurate picture of atherosclerotic risk than traditional cholesterol measurements alone. Each LDL particle contains one apo-B protein, making the apo-B count a direct measure of the number of potentially harmful particles in the bloodstream.
This distinction is critical because two people can have identical LDL cholesterol levels while having vastly different numbers of LDL particles. The person with more particles—even at the same cholesterol level—faces significantly higher cardiovascular risk. It’s not just about how much cholesterol you have; it’s about how it’s packaged and transported through your arteries.
The implications of this oversight extend far beyond academic interest. Patients with normal-appearing cholesterol profiles may harbor elevated apo-B levels, indicating a substantially higher risk of heart attack and stroke than their standard lipid panel suggests. Without proper testing, these individuals remain unaware of their true cardiovascular vulnerability.
This knowledge gap becomes even more concerning when considering inherited cholesterol disorders. Genetic variations can cause elevated apo-B levels that don’t necessarily translate to abnormal traditional cholesterol readings. These inherited risk factors can silently increase heart disease risk across generations, often going unrecognized until a cardiac event occurs.
The medical community is increasingly recognizing that comprehensive cardiovascular risk assessment requires looking beyond the standard lipid panel. Advanced testing that includes apo-B measurements, along with other emerging biomarkers, provides a more complete picture of an individual’s true risk profile.
For patients, this evolving understanding underscores the importance of having detailed discussions with healthcare providers about cardiovascular risk assessment. Those with family histories of heart disease, particularly cases where affected relatives had “normal” cholesterol levels, may benefit from more comprehensive testing that includes apo-B measurement.
The transition from traditional cholesterol screening to more sophisticated risk assessment represents a significant shift in preventive cardiology. As our understanding of cardiovascular disease mechanisms continues to evolve, the tools for identifying at-risk individuals become more precise and potentially life-saving.
This advancement in cardiac risk assessment offers hope for preventing the devastating surprise of heart attacks in seemingly healthy individuals. By identifying hidden risk factors that standard tests miss, healthcare providers can implement targeted interventions before irreversible damage occurs.
The message for patients is clear: normal cholesterol numbers, while encouraging, don’t tell the complete story of cardiovascular health. Working with knowledgeable healthcare providers to assess comprehensive risk factors—including those that traditional tests might miss—represents the future of heart disease prevention.